Hypertension: The Silent Pressure Within
Introduction
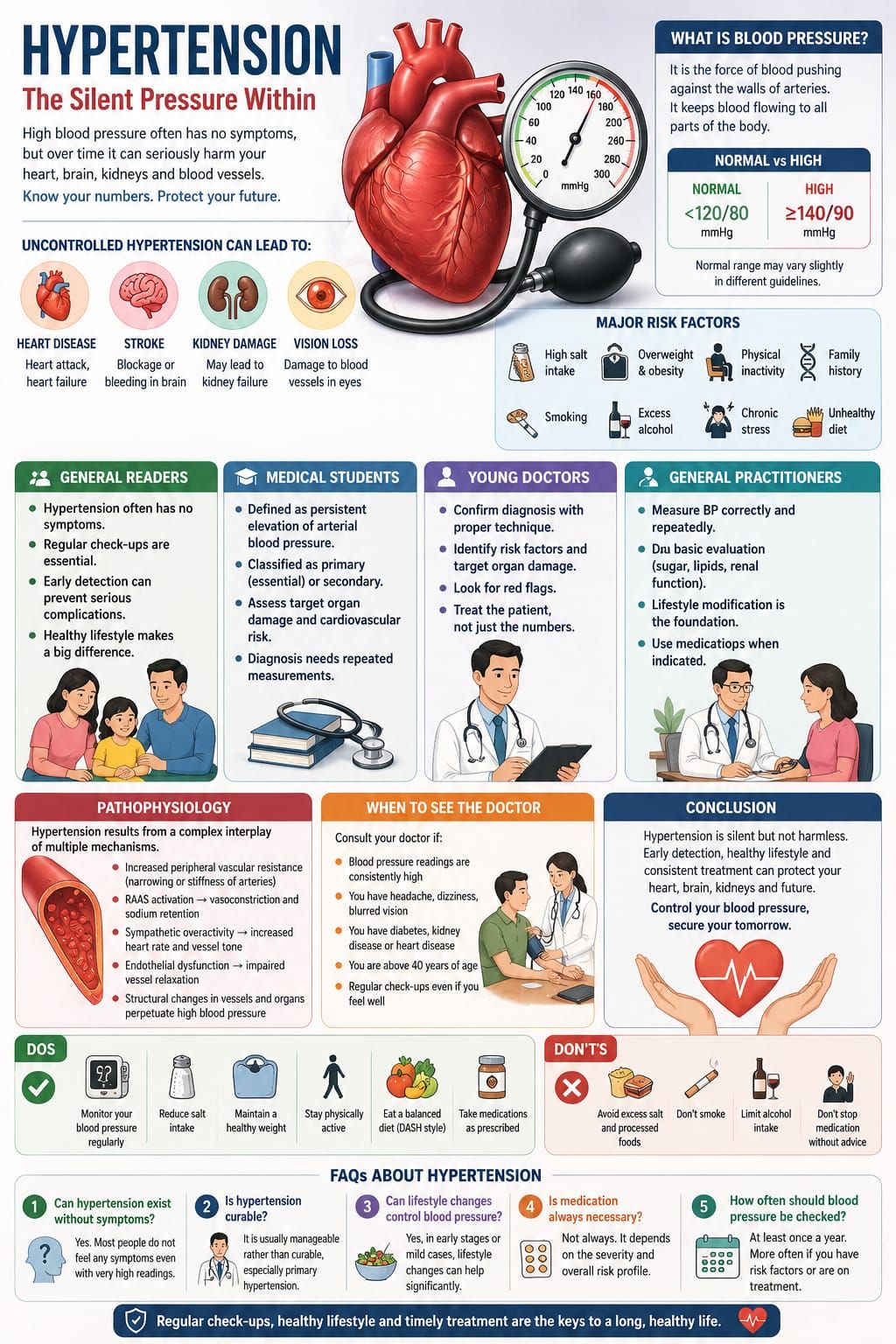
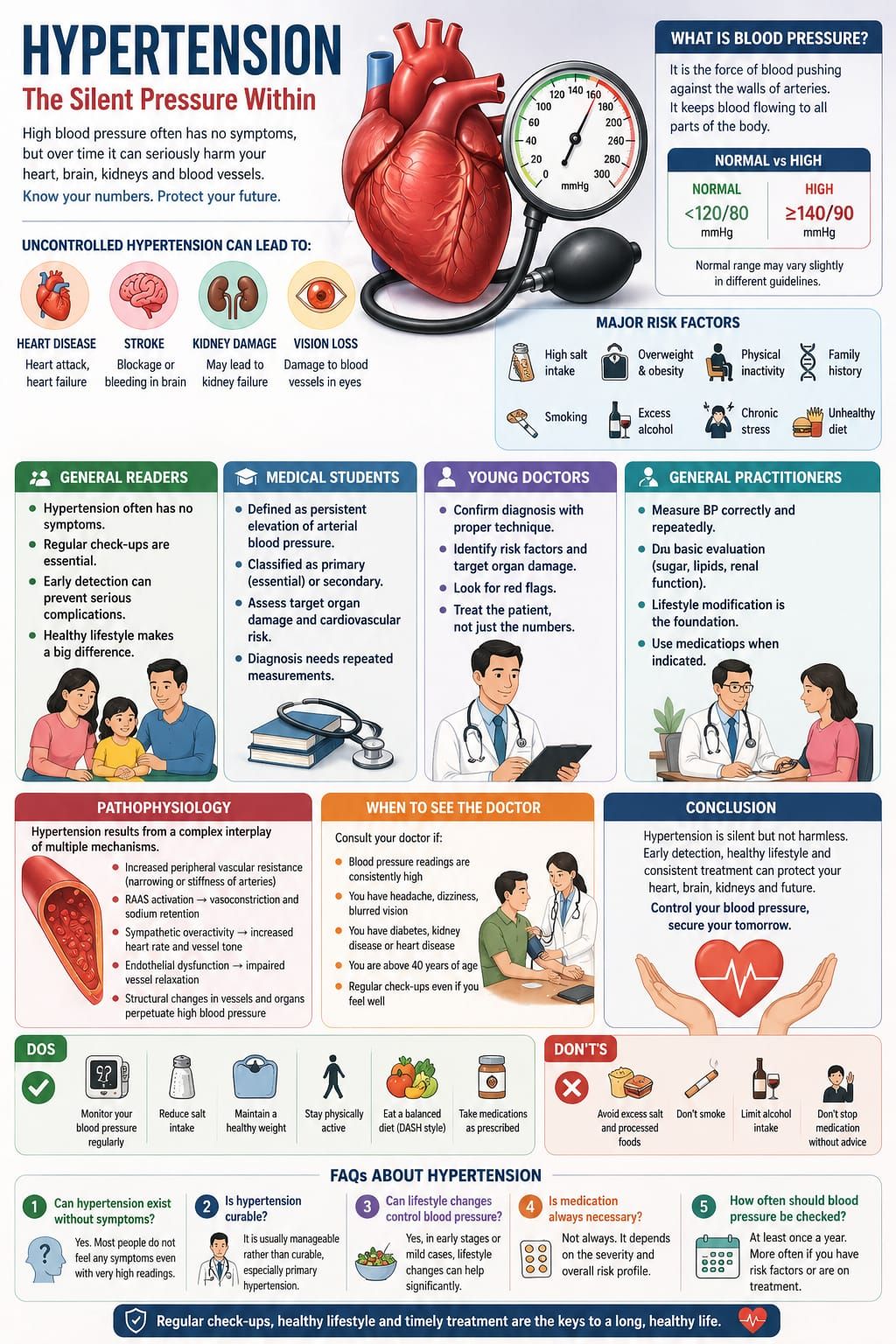
Hypertension, or high blood pressure, is one of the most common yet deceptively silent conditions encountered in medical practice. Unlike many illnesses, it often progresses without noticeable symptoms, quietly affecting vital organs over years.
For this reason, it is often referred to as the “silent killer.” The danger does not lie in how it feels—but in what it does.
Understanding hypertension is not merely about numbers on a blood pressure monitor; it is about recognizing a long-term process that influences the heart, brain, kidneys, and blood vessels.
General Readers
Blood pressure is the force with which blood pushes against the walls of arteries. It is essential for life, as it allows blood to circulate throughout the body.
However, when this pressure remains consistently elevated, it begins to harm the body.
Most people with hypertension feel completely normal. There may be no pain, no discomfort, and no warning signs. Yet, over time, high blood pressure can lead to serious problems such as:
• Heart disease
• Stroke
• Kidney damage
• Vision problems
This is why regular monitoring is crucial—even in the absence of symptoms.
Medical Students
Hypertension is defined as a persistent elevation of arterial blood pressure.
Classification (General Understanding)
• Normal
• Elevated
• Stage 1 hypertension
• Stage 2 hypertension
Types
• Primary (essential) hypertension – no identifiable cause (most common)
• Secondary hypertension – due to identifiable causes (renal, endocrine, etc.)
Key Clinical Approach
• Confirm diagnosis with repeated measurements
• Evaluate risk factors
• Screen for target organ damage
Hypertension should always be assessed in the context of the patient’s overall cardiovascular risk profile.
Young Doctors
Hypertension management requires long-term thinking rather than short-term correction.
Clinical priorities include:
• Accurate measurement (avoid single-reading diagnosis)
• Identification of risk factors:
• Obesity
• Sedentary lifestyle
• High salt intake
• Family history
• Look for subtle signs of organ involvement:
• Left ventricular hypertrophy
• Retinopathy
• Renal impairment
Avoid the common mistake of treating numbers alone—treat the patient as a whole.
General Practitioners
Hypertension is a cornerstone of primary care practice.
Practical Approach
• Measure blood pressure correctly:
• Patient relaxed
• Proper cuff size
• Multiple readings
• Basic evaluation:
• Blood sugar
• Lipid profile
• Renal function
Management Principles
• Lifestyle modification is the foundation:
• Salt restriction
• Weight control
• Regular physical activity
• Pharmacological treatment when indicated:
• ACE inhibitors / ARBs
• Calcium channel blockers
• Diuretics
Continuity of care and patient education are essential for long-term control.
Pathophysiology
Hypertension results from a complex interplay of vascular, neural, hormonal, and renal mechanisms.
Key contributing factors include:
• Increased peripheral vascular resistance
Narrowing or stiffness of blood vessels increases pressure
• Renin-angiotensin-aldosterone system (RAAS) activation
Leads to vasoconstriction and sodium retention
• Sympathetic nervous system overactivity
Increases heart rate and vascular tone
• Endothelial dysfunction
Impairs the ability of blood vessels to relax
Over time, these mechanisms lead to structural changes in blood vessels and organs, perpetuating the cycle of hypertension.
When to See the Doctor
Medical consultation is essential if:
• Blood pressure readings are consistently high
• There are symptoms such as:
• Headache
• Dizziness
• Blurred vision
• There is a history of:
• Diabetes
• Kidney disease
• Heart disease
Even in the absence of symptoms, regular check-ups are strongly advised.
Hypertension is not a condition of discomfort—it is a condition of consequence. It progresses quietly, often unnoticed, yet leaves a lasting impact on vital organs.
The key to managing hypertension lies not only in treatment but in early detection, lifestyle balance, and consistent follow-up.
For the physician, it demands vigilance.
For the patient, it requires awareness and discipline.
In controlling blood pressure, we are not just managing a number—we are protecting the future of the body.
Dos and Don’ts
Do
• Monitor blood pressure regularly
• Reduce salt intake
• Maintain a healthy weight
• Stay physically active
• Take medications as prescribed
Don’t
• Ignore high readings
• Stop medications without advice
• Consume excessive salty or processed foods
• Rely solely on symptoms for detection
FAQs About Hypertension
1. Can hypertension exist without symptoms?
Yes. Most patients remain asymptomatic for years.
2. Is hypertension curable?
It is usually manageable rather than curable, especially primary hypertension.
3. Can lifestyle changes control blood pressure?
Yes, especially in early stages or mild cases.
4. Is medication always necessary?
Not always. It depends on severity and risk factors.
5. How often should blood pressure be checked?
Regularly, especially in adults above 40 or those with risk factors.


By Dr. Mohammed Tanweer Khan
A Proactive/Holistic Physician
Founder of WithinTheBody.com