Osteoarthritis: When Joints Reflect the Passage of Time
Introduction
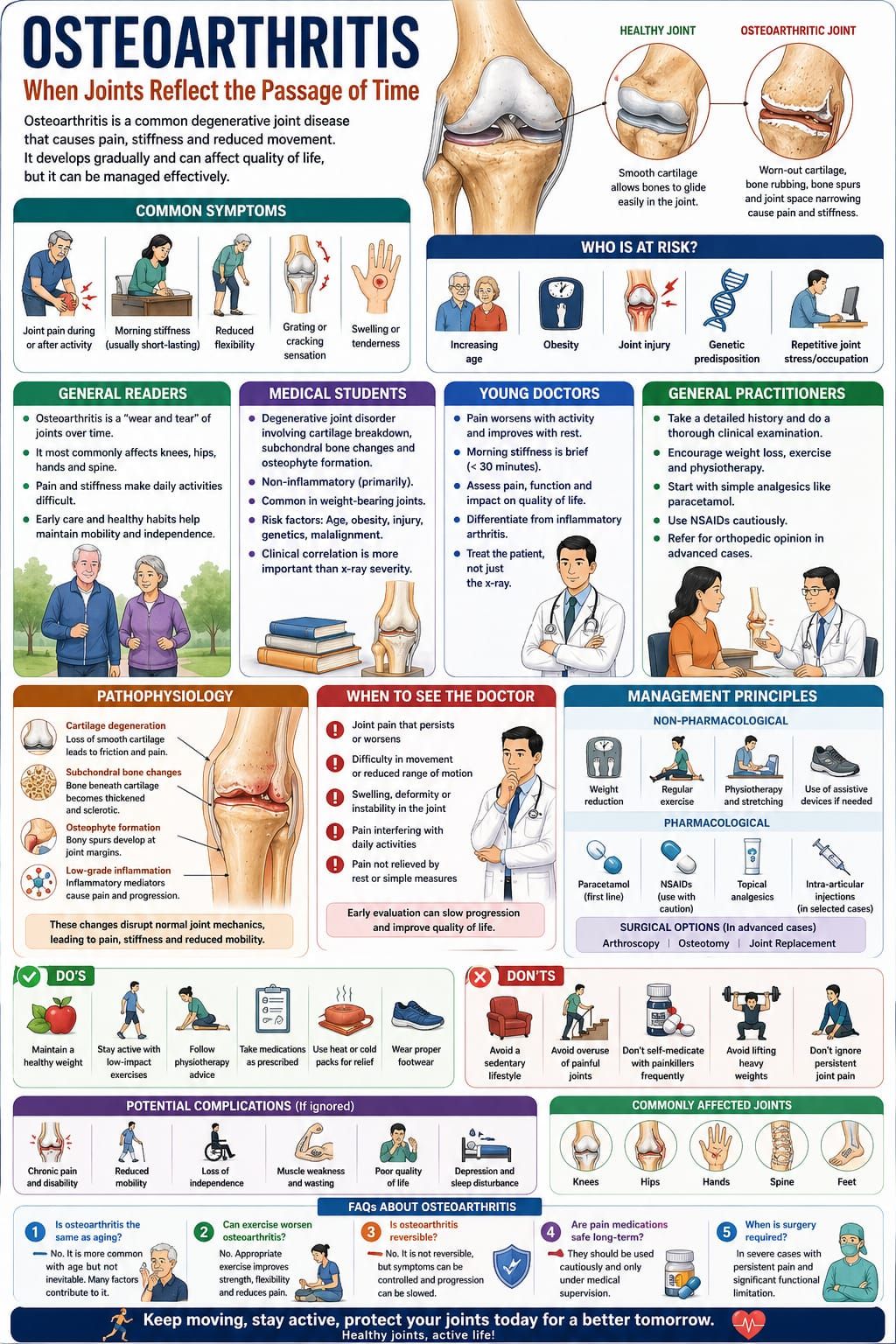
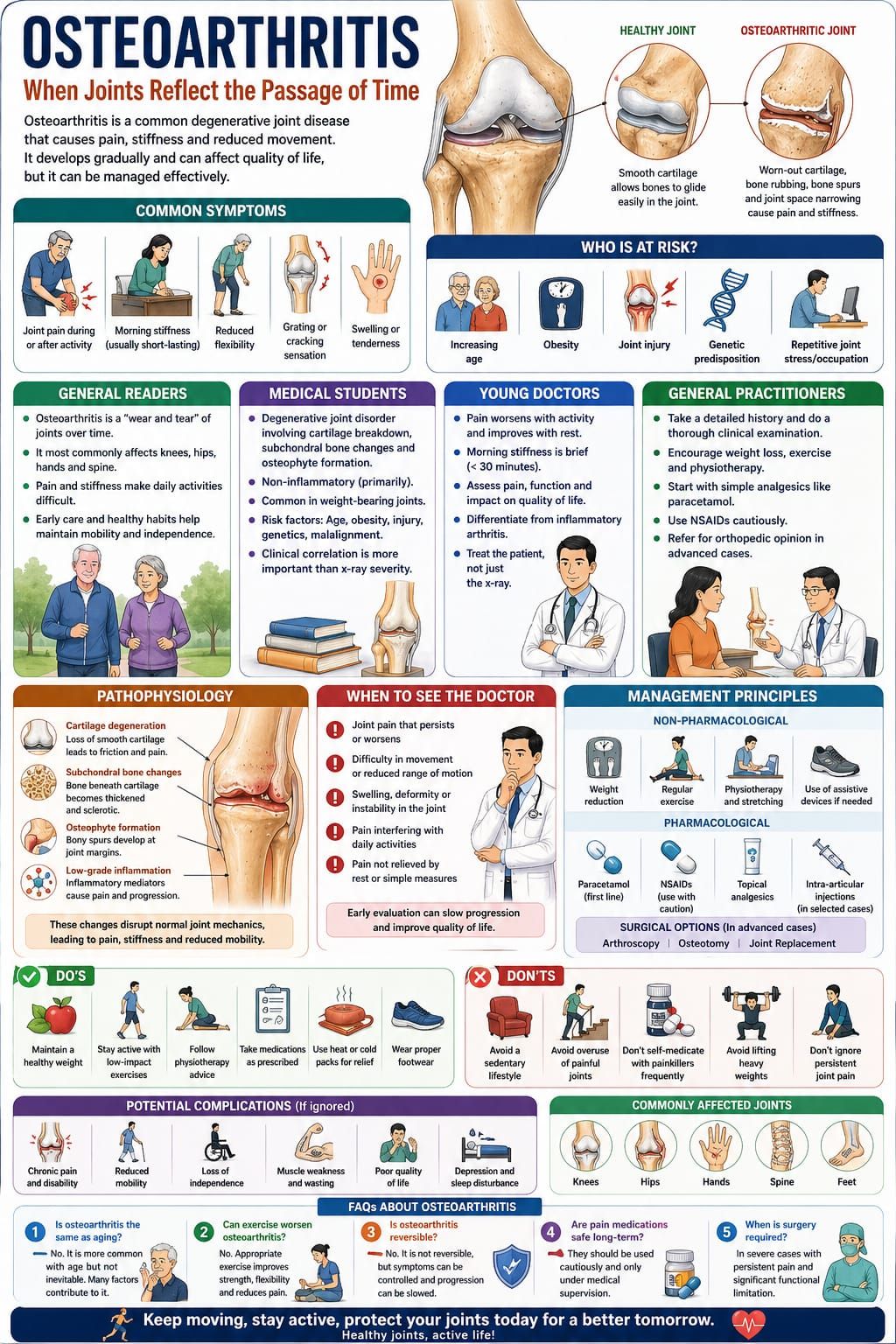
Osteoarthritis is one of the most common chronic conditions encountered in clinical practice, particularly with advancing age. It is often described as a “wear and tear” disease, but this simplification does not fully capture its complexity.
In reality, osteoarthritis represents a gradual imbalance between joint breakdown and repair. It is a condition where structure, function, and time intersect—leading to pain, stiffness, and reduced mobility.
For the physician, osteoarthritis is not merely about joints; it is about preserving movement, independence, and quality of life.
General Readers
Osteoarthritis affects the joints—the places where two bones meet, such as the knees, hips, hands, and spine.
Over time, the protective cartilage within these joints begins to wear down. As a result:
• Bones may rub against each other
• Movement becomes painful
• Joints may feel stiff, especially after rest
Common symptoms include:
• Joint pain during or after movement
• Morning stiffness (usually short-lasting)
• Reduced flexibility
• A grating or cracking sensation in joints
It develops gradually and is more common with increasing age.
Medical Students
Osteoarthritis is a degenerative joint disorder characterized by:
• Cartilage degradation
• Subchondral bone changes
• Osteophyte formation
Key Features
• Non-inflammatory (primarily)
• Commonly affects weight-bearing joints
• Progresses slowly over time
Risk Factors
• Age
• Obesity
• Joint injury
• Genetic predisposition
Radiological findings often correlate poorly with symptoms, making clinical assessment essential.
Young Doctors
In practice, osteoarthritis requires a patient-centered and functional approach.
Clinical considerations:
• Assess pain severity and functional limitation
• Do not rely solely on X-ray findings
• Differentiate from inflammatory arthritis
Important points:
• Pain typically worsens with activity and improves with rest
• Morning stiffness is brief (unlike rheumatoid arthritis)
• Joint deformity may develop in advanced cases
Management should aim at symptom relief and functional preservation.
General Practitioners
Osteoarthritis is a frequent presentation in primary care.
Practical Approach
• Detailed history:
• Duration and pattern of pain
• Effect on daily activities
• Clinical examination:
• Joint tenderness
• Range of motion
• Crepitus
Management Principles
• Non-pharmacological:
• Weight reduction
• Physiotherapy
• Exercise
• Pharmacological:
• Paracetamol
• NSAIDs (with caution)
• In advanced cases:
• Referral for orthopedic evaluation
Long-term management and patient education are key.
Pathophysiology
Osteoarthritis involves a progressive breakdown of joint structures.
Key mechanisms include:
• Cartilage degeneration
Loss of smooth articular surface leads to friction
• Subchondral bone remodeling
Bone beneath cartilage becomes thickened and sclerotic
• Osteophyte formation
Bony outgrowths develop at joint margins
• Low-grade inflammation
Contributes to pain and progression
These changes disrupt normal joint mechanics, leading to pain and reduced mobility.
When to See the Doctor
Medical consultation is necessary if:
• Joint pain persists or worsens
• Movement becomes limited
• There is swelling or deformity
• Daily activities are affected
Early evaluation helps in slowing progression and improving quality of life.
Osteoarthritis is not merely a disease of aging—it is a condition of imbalance between use and repair. It reflects the cumulative effects of time, stress, and biological change within the joints.
For the physician, the goal is not just to relieve pain, but to preserve movement and independence.
For the patient, it emphasizes the importance of maintaining activity, weight control, and joint care.
In osteoarthritis, the aim is not to reverse time—but to adapt to it wisely.
Dos and Don’ts
Do
• Maintain a healthy body weight
• Stay physically active with joint-friendly exercises
• Follow physiotherapy advice
• Use medications as prescribed
Don’t
• Ignore persistent joint pain
• Lead a sedentary lifestyle
• Overuse joints without support
• Self-medicate excessively with painkillers
FAQs About Osteoarthritis
1. Is osteoarthritis the same as aging?
No, although it is more common with age, it is not inevitable.
2. Can exercise worsen osteoarthritis?
No. Appropriate exercise actually improves joint function.
3. Is osteoarthritis reversible?
It is not reversible, but progression can be slowed.
4. Are painkillers safe for long-term use?
They should be used cautiously under medical supervision.
5. When is surgery required?
In severe cases with significant pain and functional limitation.


By Dr. Mohammed Tanweer Khan
A Proactive/Holistic Physician
Founder of WithinTheBody.com