Obesity: When Excess Weight Becomes a Disease
Introduction
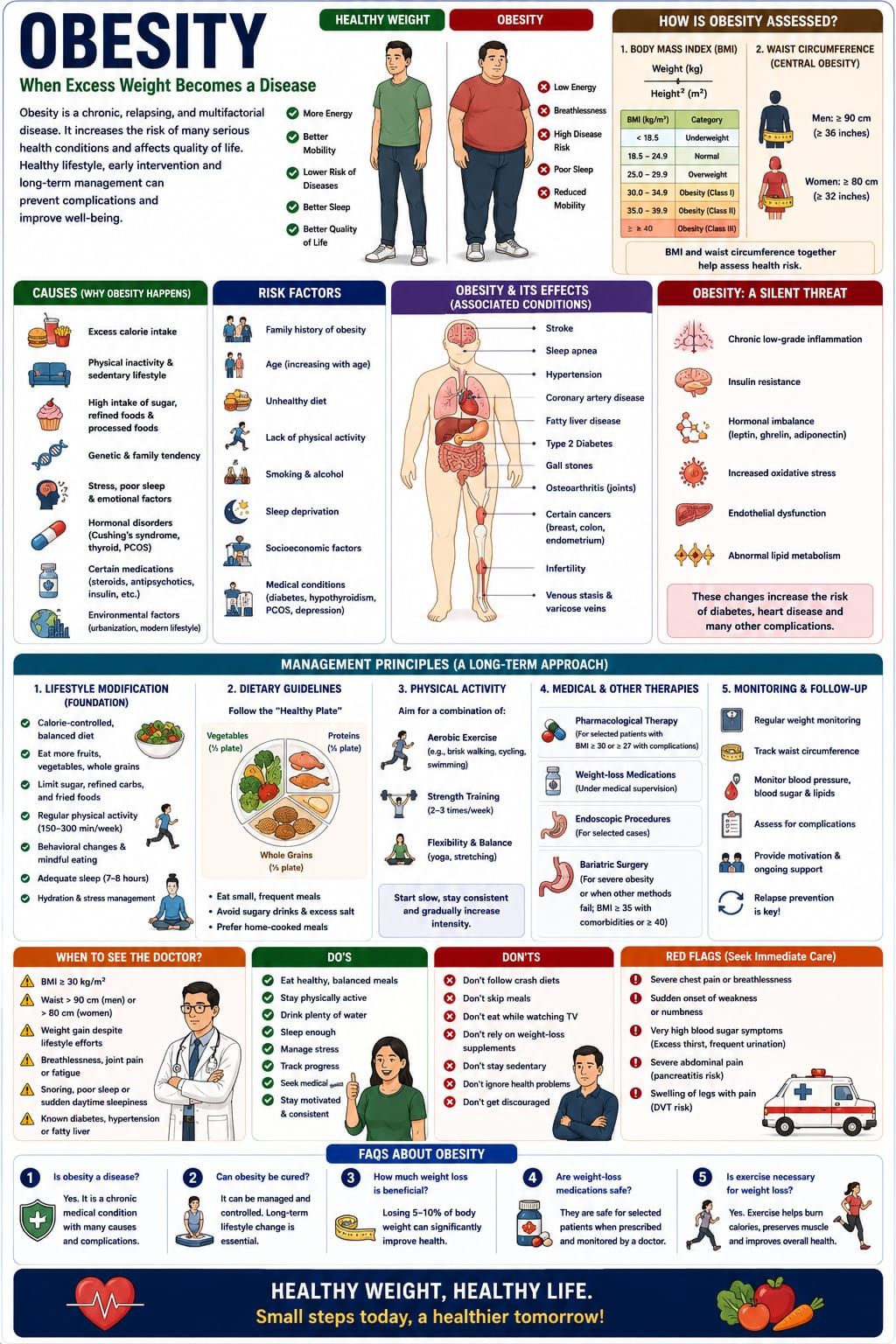
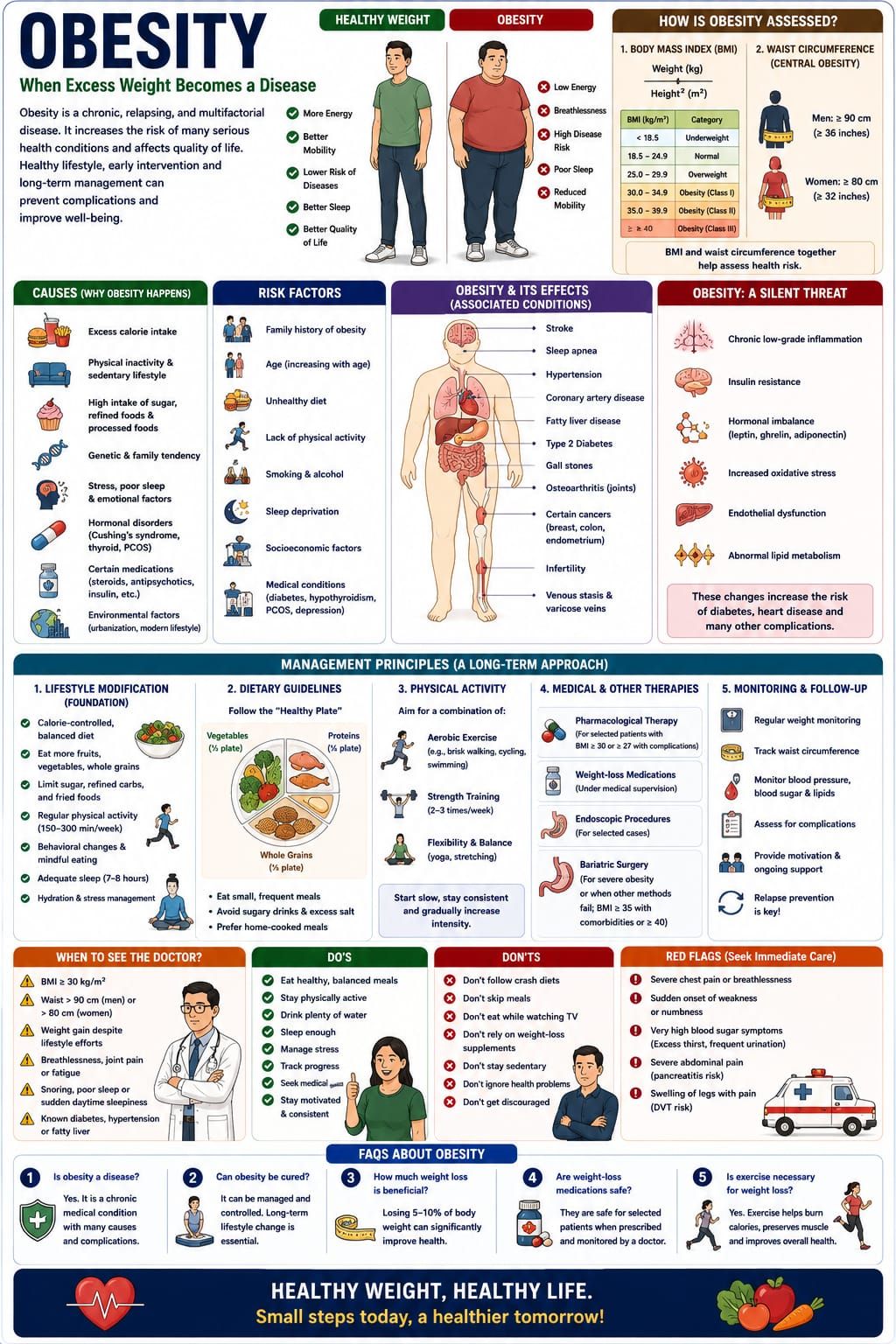
Obesity is no longer simply a matter of appearance or body shape—it is now recognized as a complex chronic disease affecting nearly every system of the body. It develops gradually, often silently, and is deeply influenced by lifestyle, environment, genetics, metabolism, and behavior.
Excess body fat does not remain biologically inactive. It alters hormonal balance, increases inflammation, and places continuous stress on vital organs. Over time, this contributes to a wide range of medical conditions including diabetes, hypertension, heart disease, sleep disorders, and joint problems.
For the physician, obesity represents not merely excess weight, but a long-term metabolic imbalance requiring comprehensive and compassionate management.
General Readers
Obesity occurs when body fat accumulates to a level that affects health.
It usually develops gradually due to:
• Excess calorie intake
• Reduced physical activity
• Sedentary lifestyle
• Poor dietary habits
Common effects of obesity include:
• Easy fatigue
• Breathlessness on exertion
• Joint pain
• Poor sleep quality
• Reduced physical mobility
Obesity also increases the risk of serious diseases such as diabetes and heart disease.
Medical Students
Obesity is defined as abnormal or excessive fat accumulation that presents a risk to health.
Assessment
• Body Mass Index (BMI)
• BMI ≥ 30 kg/m² generally indicates obesity
• Waist circumference is also important for assessing central obesity.
Key Concepts
• Multifactorial etiology:
• Genetic
• Environmental
• Behavioral
• Endocrine factors
• Adipose tissue functions as an active endocrine organ.
Obesity is associated with chronic low-grade inflammation and insulin resistance.
Young Doctors
Obesity management requires a long-term and non-judgmental approach.
Clinical priorities:
• Assess:
• BMI
• Waist circumference
• Associated comorbidities
• Evaluate for:
• Diabetes
• Hypertension
• Sleep apnea
• Fatty liver disease
Important considerations:
• Avoid blaming the patient
• Focus on sustainable lifestyle modification
• Small weight reductions can produce significant health benefits.
Behavioral counseling is often as important as medication.
General Practitioners
Obesity is increasingly common in primary care settings.
Practical Approach
• Assess dietary habits and physical activity
• Screen for obesity-related complications
Management Principles
• Lifestyle intervention:
• Calorie control
• Physical activity
• Sleep improvement
• Behavioral support and motivation
• Pharmacological or surgical options in selected patients
Long-term follow-up is essential because relapse is common.
Pathophysiology
Obesity results from chronic imbalance between energy intake and energy expenditure.
Key mechanisms include:
• Excess caloric intake
Energy stored as adipose tissue
• Insulin resistance
Commonly develops with visceral obesity
• Hormonal dysregulation
Involvement of leptin, ghrelin, and appetite pathways
• Chronic low-grade inflammation
Adipose tissue releases inflammatory mediators
These changes affect metabolism, cardiovascular health, and organ function.
When to See the Doctor
Medical consultation is necessary if:
• Weight gain becomes progressive
• There is associated diabetes or hypertension
• Breathlessness or sleep problems occur
• Daily activities become difficult
Early intervention prevents long-term complications.
Obesity is not merely excess body weight—it is a chronic metabolic condition affecting both physical and psychological health. It develops through complex interactions between biology, behavior, and environment.
For the physician, obesity care requires empathy, education, and realistic long-term planning.
For the patient, improvement begins not with rapid dieting, but with gradual, sustainable lifestyle change.
Successful management of obesity is not about perfection—it is about restoring balance and protecting long-term health.
Dos and Don’ts
Do
• Follow a balanced, portion-controlled diet
• Engage in regular physical activity
• Monitor weight regularly
• Seek professional guidance when needed
Don’t
• Follow extreme crash diets
• Depend solely on weight-loss supplements
• Lead a sedentary lifestyle
• Ignore obesity-related complications
FAQs About Obesity
1. Is obesity only due to overeating?
No. Genetics, hormones, lifestyle, and metabolism also play roles.
2. Can small weight loss improve health?
Yes. Even modest reduction improves blood pressure and sugar control.
3. Is obesity a disease?
Yes. It is now recognized as a chronic medical condition.
4. Are weight-loss medications safe?
Some may help selected patients under medical supervision.
5. When is bariatric surgery considered?
In severe obesity or when complications are significant.


By Dr. Mohammed Tanweer Khan
A Proactive/Holistic Physician
Founder of WithinTheBody.com