Fatty Liver Disease: When Fat Begins to Accumulate in the Liver
Introduction
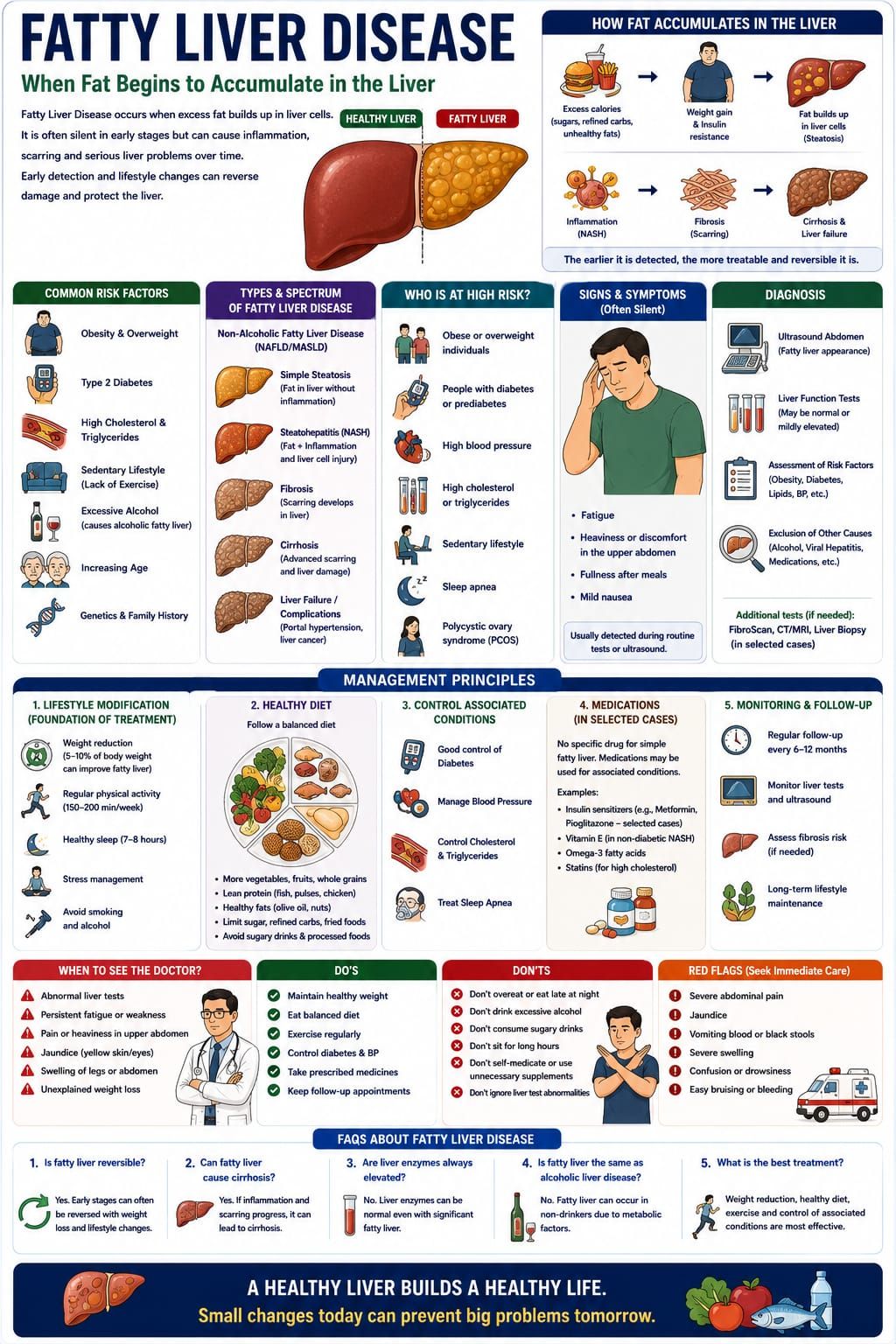
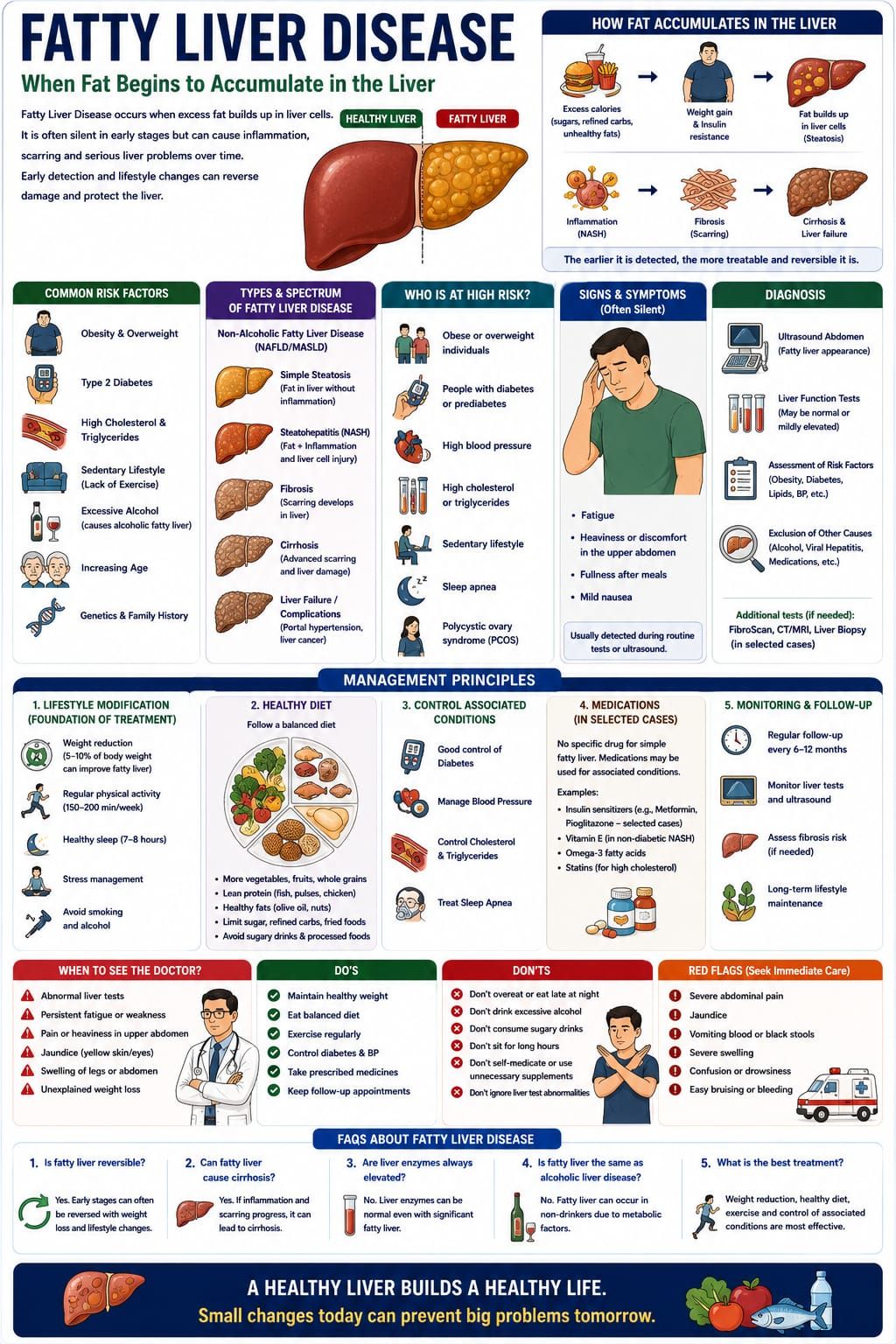
The liver is one of the most vital metabolic organs of the body. It processes nutrients, stores energy, detoxifies harmful substances, and regulates numerous biochemical functions essential for life.
Fatty Liver Disease develops when excessive fat begins to accumulate within liver cells. In its early stages, this process may remain silent and harmless-looking, but over time, persistent fat accumulation can trigger inflammation, fibrosis, and progressive liver damage.
In modern clinical practice, Fatty Liver Disease has become increasingly common, closely linked with obesity, diabetes, sedentary lifestyle, and metabolic imbalance.
For the physician, it represents not merely a liver disorder, but a systemic metabolic condition requiring early recognition and lifestyle-centered management.
General Readers
Fatty Liver Disease occurs when too much fat collects inside the liver.
Many people remain unaware of it because early stages often produce no symptoms. Some individuals may experience:
• Fatigue
• Mild discomfort in the upper abdomen
• Feeling of heaviness after meals
The condition is commonly associated with:
• Obesity
• Diabetes
• High cholesterol
• Lack of physical activity
In many cases, it is detected incidentally during ultrasound or blood tests.
Medical Students
Fatty Liver Disease includes:
• Non-Alcoholic Fatty Liver Disease (NAFLD)
• Metabolic dysfunction-associated fatty liver disease (current evolving terminology)
Spectrum
• Simple steatosis
• Steatohepatitis (NASH)
• Fibrosis
• Cirrhosis
Key Concepts
• Strong association with insulin resistance
• Hepatic fat accumulation >5% of liver weight
• Often asymptomatic initially
Liver enzymes may be normal despite significant disease.
Young Doctors
Fatty Liver Disease requires a metabolic and preventive approach.
Clinical priorities:
• Assess:
• Obesity
• Diabetes
• Lipid profile
• Hypertension
Important considerations:
• Rule out alcohol-related and secondary causes
• Ultrasound is commonly used for detection
• Weight reduction remains the cornerstone of therapy
Do not underestimate the long-term risk of fibrosis and cardiovascular disease.
General Practitioners
Fatty Liver Disease is increasingly encountered in routine practice.
Practical Approach
• Identify high-risk individuals:
• Obese patients
• Diabetics
• Patients with metabolic syndrome
• Basic evaluation:
• Liver function tests
• Ultrasound abdomen
Management Principles
• Lifestyle modification:
• Weight reduction
• Dietary correction
• Exercise
• Control associated conditions:
• Diabetes
• Hypertension
• Dyslipidemia
Patient motivation and long-term follow-up are crucial.
Pathophysiology
Fatty Liver Disease develops through metabolic imbalance and hepatic fat accumulation.
Key mechanisms include:
• Insulin resistance
Increases fat delivery to the liver
• Hepatic fat accumulation (steatosis)
Excess triglyceride storage within hepatocytes
• Oxidative stress and inflammation
Leads to liver cell injury
• Fibrosis formation
Chronic inflammation promotes scarring
Over time, persistent injury may progress to cirrhosis.
When to See the Doctor
Medical consultation is necessary if:
• There is obesity or diabetes with abnormal liver tests
• Ultrasound suggests fatty liver
• Persistent fatigue or abdominal discomfort occurs
• There are signs of advanced liver disease:
• Swelling
• Jaundice
• Unexplained weakness
Early intervention significantly improves outcomes.
Fatty Liver Disease reflects a deeper metabolic imbalance within the body. What begins as silent fat accumulation may gradually evolve into inflammation and structural liver damage if ignored.
For the physician, management extends beyond liver enzymes to addressing the entire metabolic profile.
For the patient, the most effective treatment remains lifestyle correction—particularly weight control, physical activity, and dietary balance.
The liver possesses remarkable capacity for recovery, especially when intervention begins early.
Dos and Don’ts
Do
• Maintain healthy body weight
• Exercise regularly
• Control diabetes and cholesterol
• Follow a balanced diet
Don’t
• Ignore abnormal liver tests
• Consume excessive sugary and processed foods
• Lead a sedentary lifestyle
• Use unnecessary medications or supplements excessively
FAQs About Fatty Liver Disease
1. Can fatty liver occur in non-drinkers?
Yes. Non-alcoholic fatty liver disease is very common.
2. Is fatty liver reversible?
Early stages are often reversible with lifestyle changes.
3. Can fatty liver lead to cirrhosis?
Yes, especially if inflammation and fibrosis develop.
4. Are liver enzymes always elevated?
No. Significant disease may exist with normal enzymes.
5. What is the best treatment for fatty liver?
Weight reduction and lifestyle modification remain most effective.


By Dr. Mohammed Tanweer Khan
A Proactive/Holistic Physician
Founder of WithinTheBody.com